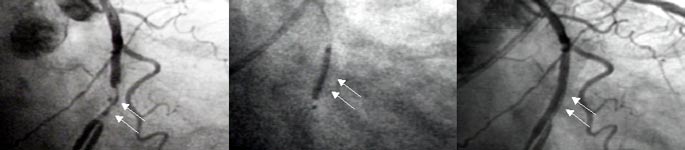
Coronary angioplasty
is a procedure used to treat angina and coronary artery disease. Much
like a cardiac catheterization a small tube or catheter is placed in an
artery, usually from the leg but occasionally from the wrist. An angioplasty
is often performed after a cardiac catheterization is done revealing serious
narrowing in the coronary arteries.
Patients are most often referred for angioplasty after presenting with an abnormal stress test, angina pectoris, unstable angina pectoris or a myocardial infarction (MI or heart attack). In general narrowing of the lumen of the coronary artery must be at least 70% before an angioplasty is considered. A guiding catheter is placed into the coronary artery and an angiogram is taken. A small wire is chosen and is placed down the artery past the narrowing, over which a deflated balloon is passed and positioned across the blockage, and is then inflated compressing the blockage into the wall. Patients may feel chest pain during balloon inflations which are performed for seconds to minutes. If the artery is opened and blood flow is near normal the balloon and wire are removed and a final angiogram is taken.
Patients are most often referred for angioplasty after presenting with an abnormal stress test, angina pectoris, unstable angina pectoris or a myocardial infarction (MI or heart attack). In general narrowing of the lumen of the coronary artery must be at least 70% before an angioplasty is considered. A guiding catheter is placed into the coronary artery and an angiogram is taken. A small wire is chosen and is placed down the artery past the narrowing, over which a deflated balloon is passed and positioned across the blockage, and is then inflated compressing the blockage into the wall. Patients may feel chest pain during balloon inflations which are performed for seconds to minutes. If the artery is opened and blood flow is near normal the balloon and wire are removed and a final angiogram is taken.